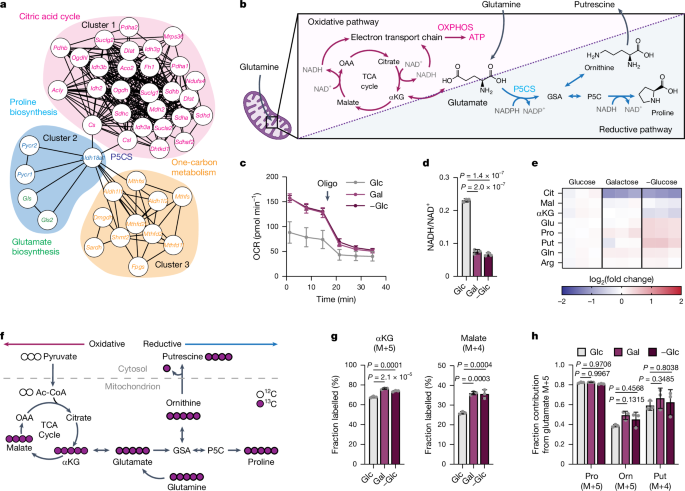
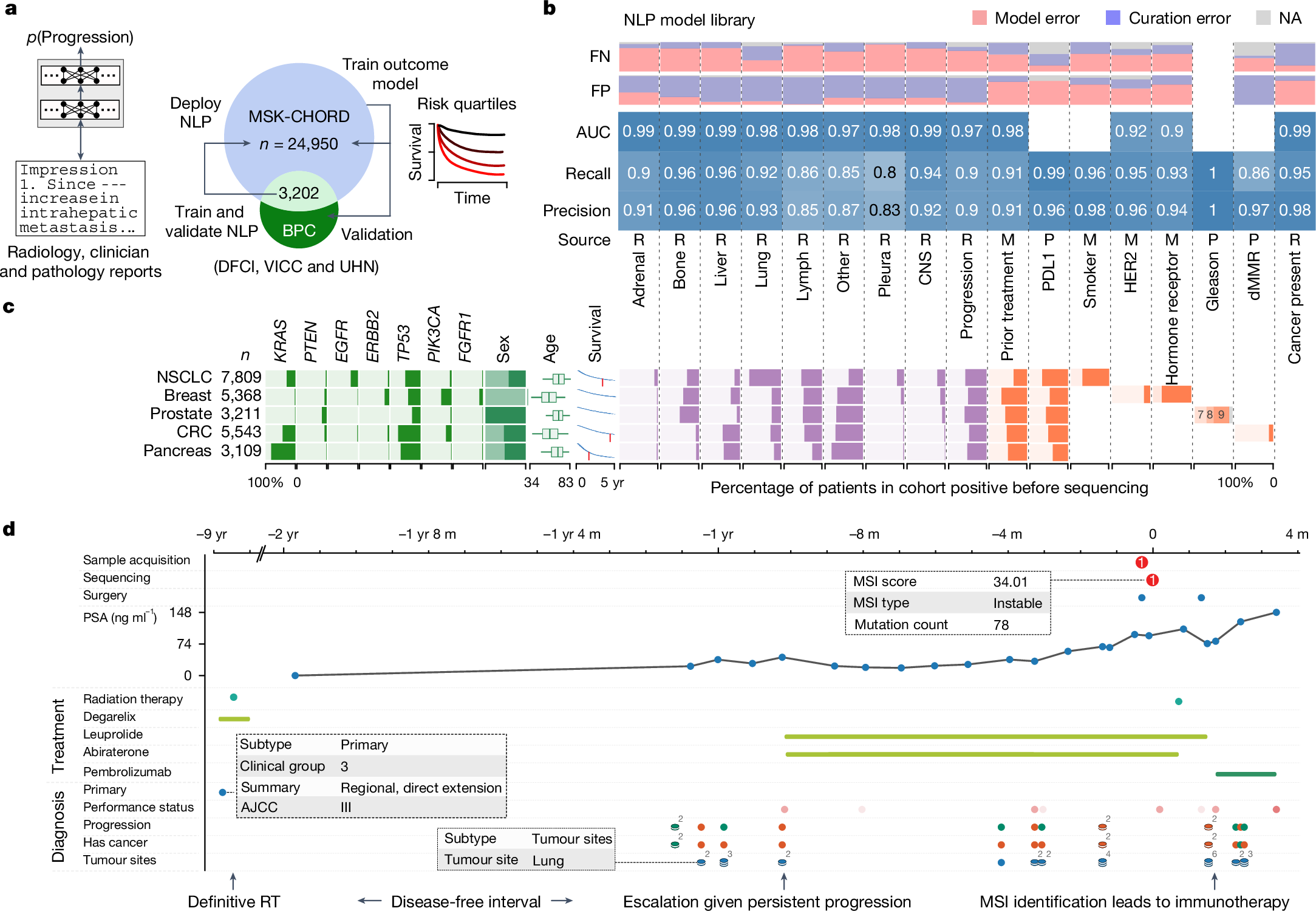
Abstract Molecular electronic devices require precise control over the flow of current in single molecules.
Charles M. is a columnist at The New York Times and a political analyst for MSNBC. He focuses on themes of medicine and healthcare, as well as social issues including racial injustice and LGBTQ rights, often intersecting these topics with current events such as the Coronavirus pandemic and the political landscape surrounding Donald Trump. Charles has been featured in numerous publications including MDPI, Nature Portfolio, and The Baltimore Sun.